“The body achieves what the mind believes.” Jim Evans
“Life is like riding a bicycle. To keep your balance, you must keep moving.” Albert Einstein

Overview: Dr. Ehlen and associates work in the Department of Neurology, Charité-University Medicine, Berlin, Germany and Faculty of Psychology and Neuroscience, Maastricht, Netherlands. Their publication is open-access and is cited as follows: Ehlen F, Schindlbeck K, Nobis L, Maier A, Klostermann F. Relationships between activity and well-being in people with Parkinson’s disease. Brain Behav. 2018; 8:e 0 0976. https://doi.org/10.1002/brb3.976
Parkinson’s is a complex disorder, this we already know. An interesting point from the paper is that usually a person-with-Parkinson’s (PwP) has reduced physical activity. We are learning that exercise is good for what ails you, especially living with Parkinson’s. Simply put, they studied how physical activity in daily life is linked to the PwP’s subjective condition (that is, their wellness, happiness, confidence, concentration, and coping strategies). This may be an obvious set of conditions, physical activity/exercise = well-being. However, their degree of sophistication and depth of evaluation makes this article interesting reading for PwP, care-partners/coaches, and health care professionals dealing with Parkinson’s.

Current understanding of Parkinson’s: The Cardinal signs (motor symptoms) of Parkinson’s include rigidity, bradykinesia (slow movement), tremor, and postural instability. Additionally, non-motor symptoms can occur, and they include depression, anxiety, apathy, dementia, impulse control disorder, and psychosis. The “quality of life” for a PwP can be dictated to some extent by the combination of motor/non-motor symptoms. As mentioned in the paper, “Health-related quality of life encompasses those aspects of well-being and satisfaction with life that affect the individual’s physical and mental health, including functional status, and social support as well as the subjective health perception (Centers for Disease Control and Prevention,2000).” This says to me that how we live with our disorder, how we cope, combine together to influence our overall health-related quality of life. A frequent by-line of this blog is to be positive and hopeful and to remain persistent; try to incorporate positive events/tasks (effects or influences) to give an edge. Like the topic here, our level of physical activity is such a positive task. We know that physical activity/exercise is good for treating Parkinson’s, and exercise counters disease-related physical inactivity. Thus, a key theme in this paper revolves around the idea that physical activity/exercise improves the patients’ (here, PwP) well-being.
Goals and Methodology: Based on the premise that physical activity/exercise is related to well-being, they tested a hypothesis that a mutual relationship exists between exercise/physical activity and the subjective condition. Furthermore, they included in their study that each person brings features that could modify this relationship like the ability to cope, personality traits and Parkinson’s symptoms.
They studied 21 PwP, and they asked them to rate their subjective condition every 2 hours and this included a self-performed description of their physical activities from the preceding 2 hour period. Clinically, they (i) measured Parkinson’s motor symptoms using the MDS-UPDRS rating scale; (ii) determined non-motor symptoms by the NonMotor Symptom (NMS) scale; (iii) the Hamilton Rating scale was used to measure depression; and (iv) the Parkinson neuropsychometric dementia assessment (PANDA) assessed Parkinson’s-related cognitive deficits. Furthermore, patients assessed themselves using (v) the Parkinson’s Disease Questionnaire (PDQ-39) for disease-specific functioning and quality of life; (vi) the Fatigue Severity Scale (FSS) to understand Parkinson’s-related fatigue, (vii) the self-assessment of the MDS-UPDRS to better describe motor and non-motor symptoms; (viii) the brief-COPE to assess the individual use of different coping strategies; and (ix) the NEO Five-Factor Inventory (NEO-FFI) to evaluate five personality factors. They asked the patients to evaluate their subjective condition during 2 weekdays of normal routine, every 2 hours of their waking time (9 assessment points per day). The evaluations focused on relevant motor and non-motor Parkinson’s symptoms. See Table below for representative terms being evaluated.
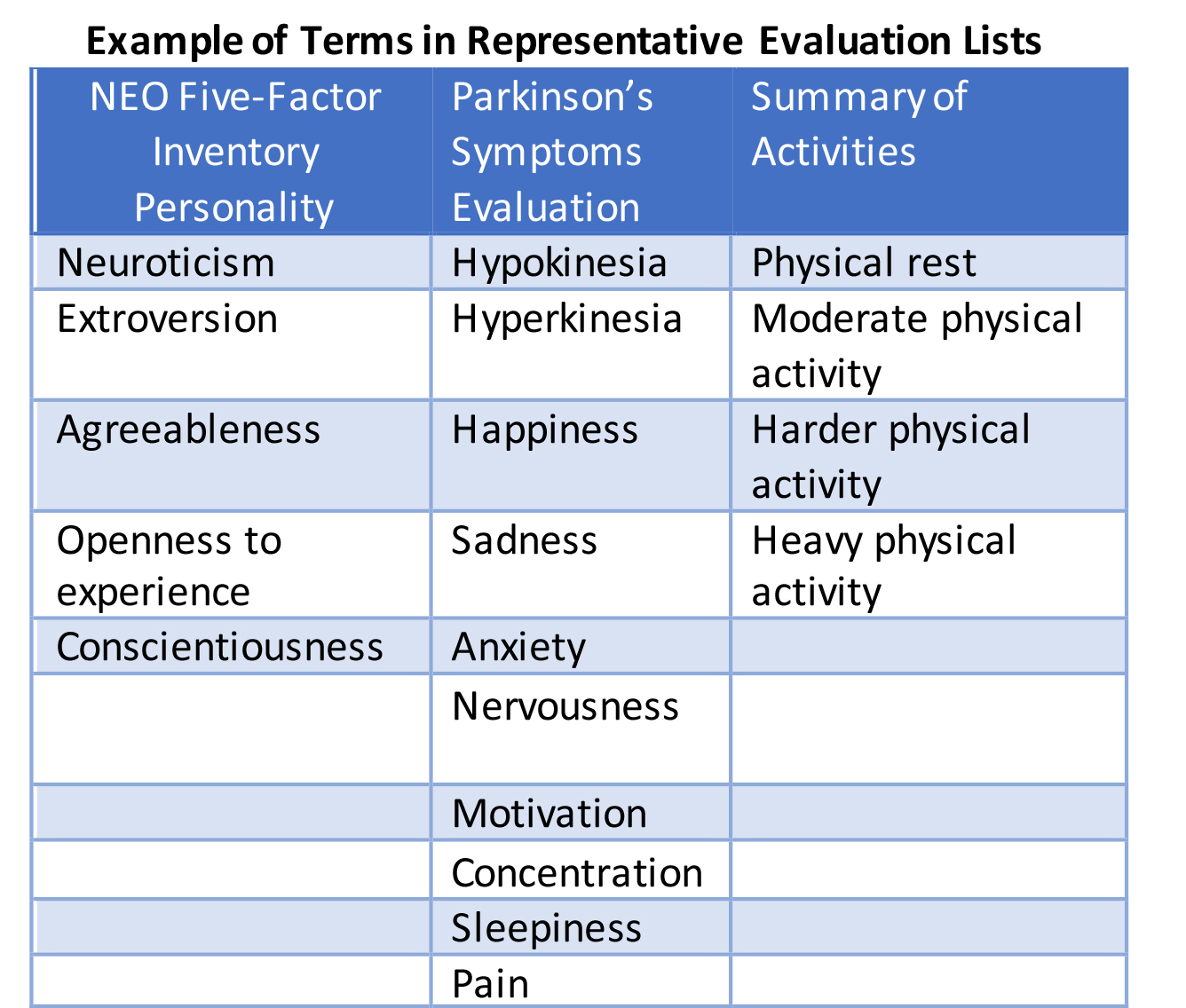
Translating/Explaining the Results: The description of the patients being studied seem very typical for Parkinson’s (i.e., demographics, therapy regimen, motor symptoms exhibited, several with depression). The so-called positive condition (happiness, motivation and concentration) was rated as 5.31 (10-point scale) and the negative condition (sleepiness, hypokinesia, nervousness, pain, anxiety and sadness) as 2.60 (again, on a 10-point scale). All of the surveys were assessed by stepwise mutivariate linear regression analyses (MRAs) in two areas: first, between the subjective condition and the duration of subsequent physical activities; and second, between physical activities and the related change in condition. From here, they performed further statistical analyses attempting to find associations with personal factors. Here is what they found out from their statistical analyses:
- The ‘positive condition’ was a highly significant predictor for performing moderate physical activity, and it was also significant for the duration of harder physical activity.
- The ‘duration’ of moderate physical activity was a highly significant predictor for an increase in positive condition.
- There was a signficant positive relationship between moderate physical activity and positive condition when including the coping factors (positve reframing, active coping, venting, planning) especially when combined with some key personality factors (which include agreeableness, conscientiousness, openness to experience, and extroversion).
- There was not a statistical significance betwen clinical scores (Parkinson’s symptoms) and time spent being physically active.
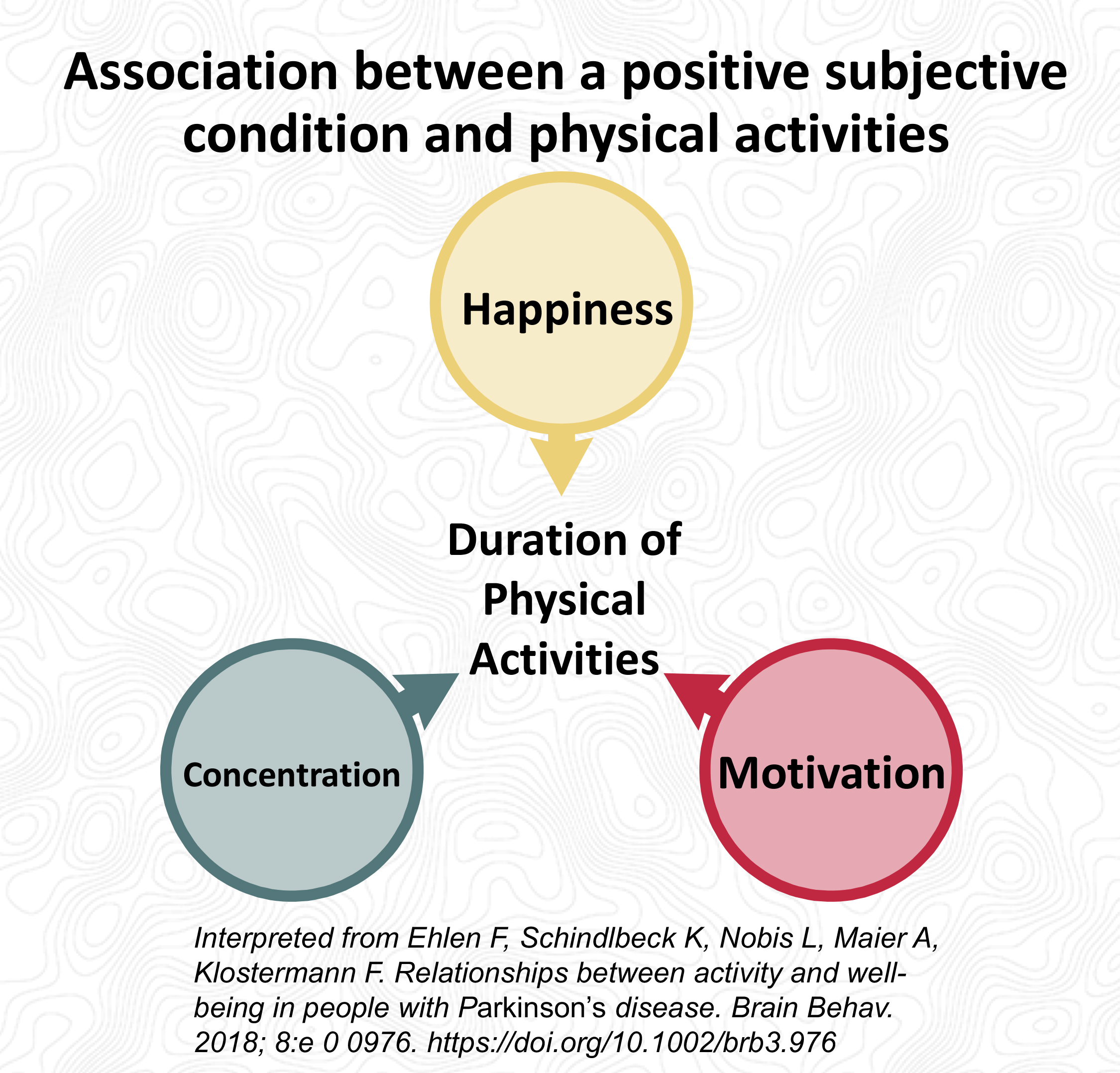
Conclusions (importance/relevance to Parkinson’s today and our future): The key result from this study was that frequent physical activity/exercise resulted in an immediate improvement in the subjective condition of PwP. There appears to be a positive feedback loop between physical activity and the subjective condition (see figure below).

Interpreting the results show that increasing the activity on an every day basis had the biggest effect on the subjective condition, i.e., exercise or do some physical activity every day. The authors also reflect that the reverse situation should be expected between physical rest and a negative subjective conditions. This indicates that inactivity should be avoided, which is at times difficult due to the sedative effects of some Parkinson’s medication.
In trying to summarize their results, they showed there is a relationship between a positive subjective condition (such as happiness, motivation and concentration) with the duration of physical activity. Get started and your quality of life will improve (see Figure below). Furthermore, they found that physical activity/exercise and improved subjective condition was most evident in patients that used positive reframing and active coping strategies with the personality traits of agreeableness, openness, conscientiousness and extroversion (see Figure below). It should be mentioned the types of physical activities the PwP reported in their log, and this included physical rest (resting, watching TV, reading or doing needlework), moderate physical activity (tidying, other household labor and walking outside), harder physical activities (bicycling, gymnastics, other sports, doing garden work) and heavy physical work (shoveling snow and chopping wood).
Get up and get going every day. The goal is to do some exercise/physical activity, and your quality of life will show an immediate improvement. It is also essential for our health care providers to encourage us to commit to exercise/physical activity.
“Physical fitness takes commitment to exercise just as it requires good nutrition. But it doesn’t have to be painful. Just the opposite: Vigorous exercise actually is stimulating. It boosts your energy levels, invigorates your mind, and just feels good afterward. The hardest part, of course, is getting started.”Jack LaLanne
Cover photo credit: http://baycolonyjunobeach.com/project/juno/




beautiful insightful thank you!
LikeLike
Thank you, Frank
LikeLike