“To the sick, while there is life there is hope. [Lat., Aegroto dum anima est, spes est.]” Marcus Tullius Cicero
“We can’t live without hope. When we keep hoping, we keep living.” Pete Wilson
Introduction: Palmitoylethanolamide (PEA*) is a naturally occurring bioactive lipid that contains a fatty acid moiety and ethanolamide. The molecular formula of PEA is C18H37NO2, and the chemical structure of Palmitoylethanolamide (PEA) is shown below.
Recently, I posted a blog on the potential role of PEA in treating Parkinson’s: “Role of Palmitoylethanolamide to Control Neuroinflammation and Potential Therapy for Parkinson’s.” I started using it more than five months ago (July 2022), and I am convinced it is helping me deal with my Parkinson’s symptoms. Since I am only an n = 1, my results do not matter much. However, I know that several of you are also taking PEA, that is, palmitoylethanolamide. Thus, the new material is for everyone’s further understanding of PEA.
In this blog post, (a) I have included some safety and efficacy studies with PEA, (b) comparing PEA to micronized to ultra-micronized PEA and treating various disorders, including those related/linked to Parkinson’s, and (c) my current use and experiences with PEA [Please refer to the first post on PEA and Parkinson’s for additional insight and information (“Role of Palmitoylethanolamide to Control Neuroinflammation and Potential Therapy for Parkinson’s.”)]. A list of references (separated by section topics) is included at the end of the blog post.
*Please note the PEA discussed in this blog post is palmitoylethanolamide (also known as N-palmitoylethanolamine). Importantly, it is NOT to be confused with Phenylethyl Alcohol (also abbreviated PEA) or the protein extracted from field peas (Scientific name: Pisum sativum).
“I’ve always said that you can live without water for many days, but you can’t live for a second without hope.” Brendan Rodgers
PEA Mechanism of Action in Inflammation/Neuroinflammation: PEA is considered a bioactive lipid amide, which is synthesized and sequestered into the cell lipid bilayer of the surface. Significantly, PEA synthesis increases in response to cellular injury. Thus, it is a modulating substance made by a cell in response to injury. PEA has many different biological actions. PEA is a ligand that activates the nuclear receptor, peroxisome proliferator-activated receptor-α (PPAR-α), which supports an anti-inflammatory activity. PEA also binds to the cannabinoid-like G-coupled receptors GPR55 and GPR119.
Interestingly, GPR55 is widely expressed in many areas of the brain. However, due to its overall effect to be a mediator of the resolution of inflammatory methodologies, PEA can be considered a maintenance factor for cellular homeostasis. Furthermore, since neuroinflammation is one of the critical mediators of Parkinson’s, down-regulating this inflammatory process may be an essential ingredient for the therapeutic potential of PEA in treating Parkinson’s. And the literature has shown that PEA does penetrate the blood-brain barrier.
“While there’s life, there is hope.” Stephen Hawking
PEA Safety and Efficacy: PEA has been studied since the 1970s in more than 30 clinical trials involving 6,000 patients. Thus, significant data suggests that taking PEA is safe for human consumption. Typically, patients have received >600 mg of PEA twice per day for several months and then, from 6-12 months, reduced the amount to >600 mg PEA per day. Long-term use of PEA has not been performed past 12 months. In a synopsis of these articles, it would appear that no damage is reported to the liver and kidneys with treatment with PEA. In addition, PEA has been tested in many clinical settings for numerous inflammatory-related disorders. Most of these studies conclude that PEA is safe as an adjunctive agent to be utilized alongside other medications.
“When you have lost hope, you have lost everything. And when you think all is lost, when all is dire and bleak, there is always hope.” Pittacus Lore
PEA (+/- Luteolin) for Treating Neurodegenerative Disorders: These two blog posts about PEA revolve around the clinical trial for Parkinson’s performed by Brotini et al. (2017).
A summary of this study- MDS-UPDRS clinical assessment was carried out monthly for three consecutive months before the actual trial began. After that, um (ultra-micronized)-PEA at 1200 mg um-PEA/day was added to levodopa therapy for three months. In the fourth month, the dose was reduced to 600 mg/day of um-PEA for up to 12 months. Using the Hoehn and Yahr (HY) Scale to determine the severity of Parkinson’s showed these changes, going from 1.8 ± 0.23 three months before the study to 2.5 ± 0.14 at the start of the clinical research. After a year of um-PEA therapy, the collective HY score was 1.9 ± 0.15. Remarkable results.
Luteolin– Several studies have added a flavonoid compound with PEA to further reduce neuroinflammation. The substance most tested was luteolin. In the works, I am preparing a blog post dedicated to luteolin because it is growing in use for anti-inflammatory processes. Luteolin, 3′,4′,5,7-tetrahydroxyflavone, is a flavonoid found in many plants, including fruits, vegetables, and medicinal herbs. Like PEA, luteolin crosses the blood-brain barrier. Furthermore, the activities of PEA and luteolin are complementary. This suggests that using PEA and luteolin to control neuroinflammation in Parkinson’s and other neurodegenerative disorders may be preferred.
“It was better to live with disappointment and frustration than to live without hope.” Robert A. Heinlein
PEA Micronized and Ultra-micronized: PEA is a lipid (fatty acid amide), and as a powder, it does not dissolve in most things we eat or drink. Thus, to increase the ‘bioavailability’ of the generally large particles, scientists prepared micronized (m-PEA) and ultra-micronized PEA (um-PEA). The results suggest that um-PEA and m-PEA are more effective than PEA; however, much work still needs to be performed for a conclusion. The chemical content of PEA is unchanged; it is just the size of the particles generated by micro- and ultra-micronization. Regarding safety, the micronized/ultra-micronized forms of PEA are as safe as PEA. For a comprehensive review, please see Nestmann (2016) for details about safety and toxicity results for the various forms of PEA. The multiple forms of PEA are safe for humans to use for at least 12 months. Schweiger et al. (2019) reported good treatment response with ultramicronized-PEA in fibromyalgia syndrome for up to 15 months. And <15% of the patients reported adverse effects related to gastrointestinal discomfort from the PEA (diarrhea, dyspepsia, bloating, constipation, vomiting) [NOTE: I only have access to the Abstract].
“As long as we can feel hope, there is hope.” Harriet Lerner
My Strategy and Results with PEA: I have used various PEA products under the following scenarios.
Types of PEA- It is essential to mention that I continue to take Carbidopa/Levodopa and the Neupro dopamine agonist patch daily. And the dose and timing of taking them have not changed for the past year and seven months. Thus, my reasons for taking PEA were for an adjunctive role in maintaining the health of remaining dopaminergic neurons and, in general, to reduce the neuroinflammatory environment that likely exists in my brain.
Table 1 below describes the types of PEA products utilized.

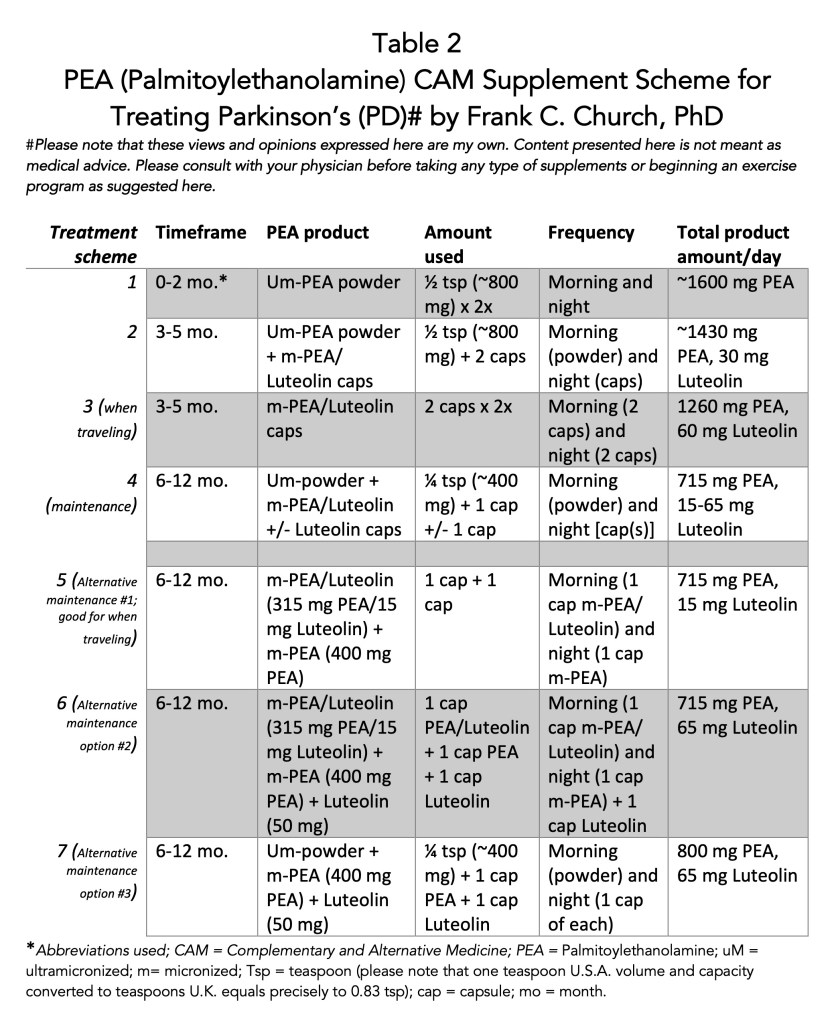
Protocol Followed with PEA- Table 2 below shows how I have used the PEA products for the last five months. And below Table 2, I have depicted the three types of PEA being described and used here.
I have used several derivatives of PEA. First, I started using the powder form of um-PEA, taking 800 mg PEA twice daily. Then, at the start of the third month, I combined the powder um-PEA with the m-PEA/Luteolin capsules to take 1430 mg PEA daily with 30 mg Luteolin. At the start of 2023, I will migrate to a maintenance schedule. The plan includes reducing the amount of PEA to 715-800 mg daily. The significant variables will be deciding which form of PEA to use and how much luteolin to take. Please use Table 2 as a detailed guide to my past, current, and future use of PEA.
My Personal Experience with Palmitoylethanolamide (PEA)*– Adding PEA to my daily regimen has positively impacted my health. I am not as anxious, and my everyday mood has improved. I am sleeping better and able to turn over in bed a little better. My body pain levels seem lower than before, and my daytime sleepiness has improved. I have not had problems with dressing, walking, balance, or freezing, so that’s not changed. My overall motor functions seem more stable, if not slightly improved. There have been days when I skipped my last dose of carbidopa/levodopa and did not regret it when I woke up the following day, an exciting feeling.
Undoubtedly, I need carbidopa/levodopa to help reduce my stiffness and flexibility and control my tremor. However, I feel that using PEA has been beneficial to my overall health with Parkinson’s. Thus, I will continue with PEA for the next six months and stay hopeful that the changes remain.
*Medical Disclaimer: As with anything you read here, please consult your Neurologist before taking any form of palmitoylethanolamide (PEA). While it appears safe, that does not mean it is right for you to take it for your Parkinson’s.
“… combined together with hope, we continue, we live, we continue to live, and we continue to live well and strong in the presence of Parkinson’s.” Frank C. Church
References:
References for PEA Mechanism of Action in Inflammation/Neuroinflammation
Verme, Jesse Lo, Jin Fu, Giuseppe Astarita, Giovanna La Rana, Roberto Russo, Antonio Calignano, and Daniele Piomelli. “The nuclear receptor peroxisome proliferator-activated receptor-α mediates the anti-inflammatory actions of palmitoylethanolamide.” Molecular pharmacology 67, no. 1 (2005): 15-19.
Clayton, Paul, Mariko Hill, Nathasha Bogoda, Silma Subah, and Ruchitha Venkatesh. “Palmitoylethanolamide: a natural compound for health management.” International Journal of Molecular Sciences 22, no. 10 (2021): 5305.
Clayton, Paul, Silma Subah, Ruchitha Venkatesh, Mariko Hill, and Nathasha Bogoda. “Palmitoylethanolamide: A potential alternative to cannabidiol.” Journal of Dietary Supplements (2021): 1-26.
Valenza, Marta, Roberta Facchinetti, Luca Steardo, and Caterina Scuderi. “Palmitoylethanolamide and White Matter Lesions: Evidence for Therapeutic Implications.” Biomolecules 12, no. 9 (2022): 1191.
Keppel Hesselink, J. M., Tineke de Boer, and Renger F. Witkamp. “Palmitoylethanolamide: a natural body-own anti-inflammatory agent, effective and safe against influenza and common cold.” International journal of inflammation 2013 (2013).
Gatti, Antonio, Marzia Lazzari, Valentina Gianfelice, Annarita Di Paolo, Elisabetta Sabato, and Alessandro Fabrizio Sabato. “Palmitoylethanolamide in the treatment of chronic pain caused by different etiopathogenesis.” Pain Medicine 13, no. 9 (2012): 1121-1130.
Petrosino, Stefania, and Aniello Schiano Moriello. “Palmitoylethanolamide: A Nutritional Approach to Keep Neuroinflammation within Physiological Boundaries—A Systematic Review.” International Journal of Molecular Sciences 21, no. 24 (2020): 9526.
Siracusa, Rosalba, Irene Paterniti, Daniela Impellizzeri, Marika Cordaro, Rosalia Crupi, Michele Navarra, Salvatore Cuzzocrea, and Emanuela Esposito. “The association of palmitoylethanolamide with luteolin decreases neuroinflammation and stimulates autophagy in Parkinson’s disease model.” CNS & Neurological Disorders-Drug Targets (Formerly Current Drug Targets-CNS & Neurological Disorders) 14, no. 10 (2015): 1350-1366.
Skaper, Stephen D., Laura Facci, Massimo Barbierato, Morena Zusso, Giuseppe Bruschetta, Daniela Impellizzeri, Salvatore Cuzzocrea, and Pietro Giusti. “N-Palmitoylethanolamine and neuroinflammation: a novel therapeutic strategy of resolution.” Molecular neurobiology 52, no. 2 (2015): 1034-1042.
References for PEA Safety and Efficacy-
Gabrielsson, Linda, Sofia Mattsson, and Christopher J. Fowler. “Palmitoylethanolamide for the treatment of pain: pharmacokinetics, safety and efficacy.” British journal of clinical pharmacology 82, no. 4 (2016): 932-942.
Nestmann, Earle R. “Safety of micronized palmitoylethanolamide (microPEA): lack of toxicity and genotoxic potential.” Food Science & Nutrition 5, no. 2 (2017): 292-309.
Steels, Elizabeth, Ruchitha Venkatesh, Eleanor Steels, Gemma Vitetta, and Luis Vitetta. “A double-blind randomized placebo controlled study assessing safety, tolerability and efficacy of palmitoylethanolamide for symptoms of knee osteoarthritis.” Inflammopharmacology 27, no. 3 (2019): 475-485.
Hesselink, Jan M. Keppel, and David J. Kopsky. “Palmitoylethanolamide, a neutraceutical, in nerve compression syndromes: efficacy and safety in sciatic pain and carpal tunnel syndrome.” Journal of Pain Research 8 (2015): 729.
Khalaj, Mona, Amene Saghazadeh, Elham Shirazi, Mohammad-Reza Shalbafan, Kaveh Alavi, Mitera Hakim Shooshtari, Fatemeh Yousefi Laksari, Maryamalsadat Hosseini, Mohammad-Reza Mohammadi, and Shahin Akhondzadeh. “Palmitoylethanolamide as adjunctive therapy for autism: Efficacy and safety results from a randomized controlled trial.” Journal of psychiatric research 103 (2018): 104-111.
Abedini, Talieh, Reyhaneh Hosseyni, Farnaz Ghannadi, Hossein Sanjari Moghaddam, Mohammad‐Reza Khodaei Ardakani, Ali Talaei, and Shahin Akhondzadeh. “Efficacy and safety of palmitoylethanolamide as an adjunctive treatment for acute mania: A randomized, double‐blind, placebo‐controlled trial.” Psychiatry and Clinical Neurosciences 76, no. 10 (2022): 505-511.
Pickering, Emily, Elizabeth L. Steels, Kathryn J. Steadman, Amanda Rao, and Luis Vitetta. “A randomized controlled trial assessing the safety and efficacy of palmitoylethanolamide for treating diabetic-related peripheral neuropathic pain.” Inflammopharmacology (2022): 1-15
References for PEA (+/- Luteolin) for Treating Neurodegenerative Disorders-
Beggiato, Sarah, Maria Cristina Tomasini, and Luca Ferraro. “Palmitoylethanolamide (PEA) as a potential therapeutic agent in Alzheimer’s disease.” Frontiers in pharmacology 10 (2019): 821.
Brotini, Stefania, Carlo Schievano, and Leonello Guidi. “Ultra-micronized palmitoylethanolamide: an efficacious adjuvant therapy for Parkinson’s disease.” CNS & Neurological Disorders-Drug Targets (Formerly Current Drug Targets-CNS & Neurological Disorders) 16, no. 6 (2017): 705-713.
Esposito, Emanuela, Daniela Impellizzeri, Emanuela Mazzon, Irene Paterniti, and Salvatore Cuzzocrea. “Neuroprotective activities of palmitoylethanolamide in an animal model of Parkinson’s disease.” (2012): e41880.
Cordaro, Marika, Salvatore Cuzzocrea, and Rosalia Crupi. “An update of palmitoylethanolamide and luteolin effects in preclinical and clinical studies of neuroinflammatory events.” Antioxidants 9, no. 3 (2020): 216.
Paterniti, Irene, Marika Cordaro, Michela Campolo, Rosalba Siracusa, Carolin Cornelius, Michele Navarra, Salvatore Cuzzocrea, and Emanuela Esposito. “Neuroprotection by association of palmitoylethanolamide with luteolin in experimental Alzheimer’s disease models: the control of neuroinflammation.” CNS & Neurological Disorders-Drug Targets (Formerly Current Drug Targets-CNS & Neurological Disorders) 13, no. 9 (2014): 1530-1541.
Facchinetti, Roberta, Marta Valenza, Maria Rosanna Bronzuoli, Giorgia Menegoni, Patrizia Ratano, Luca Steardo, Patrizia Campolongo, and Caterina Scuderi. “Looking for a Treatment for the Early Stage of Alzheimer’s Disease: Preclinical Evidence with Co-Ultramicronized Palmitoylethanolamide and Luteolin.” International Journal of Molecular Sciences 21, no. 11 (2020): 3802.
Scuderi, Caterina, Giuseppe Esposito, Angelo Blasio, Marta Valenza, Pierluca Arietti, Luca Steardo Jr, Rosa Carnuccio et al. “Palmitoylethanolamide counteracts reactive astrogliosis induced by β‐amyloid peptide.” Journal of Cellular and Molecular Medicine 15, no. 12 (2011): 2664-2674.
Landolfo, Eugenia, Debora Cutuli, Laura Petrosini, and Carlo Caltagirone. “Effects of Palmitoylethanolamide on Neurodegenerative Diseases: A Review from Rodents to Humans.” Biomolecules 12, no. 5 (2022): 667.
Brotini, Stefania. “Palmitoylethanolamide/Luteolin as Adjuvant Therapy to Improve an Unusual Case of Camptocormia in a Patient with Parkinson’s Disease: A Case Report.” Innovations in Clinical Neuroscience 18, no. 10-12 (2021): 12.
References for PEA Micronized and Ultramicronized-
Nestmann, Earle R. “Safety of micronized palmitoylethanolamide (microPEA): lack of toxicity and genotoxic potential.” Food Science & Nutrition 5, no. 2 (2017): 292-309.
De Luca, Pietro, Angelo Camaioni, Pasquale Marra, Giovanni Salzano, Giovanni Carriere, Luca Ricciardi, Resi Pucci, Nicola Montemurro, Michael J. Brenner, and Arianna Di Stadio. “Effect of Ultra-Micronized Palmitoylethanolamide and Luteolin on Olfaction and Memory in Patients with Long COVID: Results of a Longitudinal Study.” Cells 11, no. 16 (2022): 2552.
Caltagirone, Carlo, Carlo Cisari, Carlo Schievano, Rosanna Di Paola, Marika Cordaro, Giuseppe Bruschetta, Emanuela Esposito, and Salvatore Cuzzocrea. “Co-ultramicronized palmitoylethanolamide/luteolin in the treatment of cerebral ischemia: from rodent to man.” Translational stroke research 7, no. 1 (2016): 54-69.
Schweiger, Vittorio, Alvise Martini, Paola Bellamoli, Katia Donadello, Carlo Schievano, Giovanna D. Balzo, Piercarlo Sarzi-Puttini, Massimo Parolini, and Enrico Polati. “Ultramicronized palmitoylethanolamide (um-PEA) as add-on treatment in fibromyalgia syndrome (FMS): retrospective observational study on 407 patients.” CNS & Neurological Disorders-Drug Targets (Formerly Current Drug Targets-CNS & Neurological Disorders) 18, no. 4 (2019): 326-333.
“We should do three things every day of our life. Number one is laugh. You should laugh every day. Number two is to think, we should spend some time in thought. And, number three is you should have your emotions moved to tears.” Jim Valvano
Cover Photo Image by Greg Montani from Pixabay






Frank, thanks for a very helpful post on PEA as usual. I note in Table 1 that you take thiamine HCL. May I ask what dose you are taking? I am sure you are aware of high dose thiamine therapy (HDTT) for PD used by the late Dr. Costantini and now advocated by Daphne Bryan (she has a book out on using HDTT for PD). Do you have any success with HDTT? Very interested to hear your feedback as my sister (PwP) is currently trying HDTT.
Regards,
Philip
LikeLike
Philip, thanks for your note. I was saddened by Dr. Costantini’s passing; he was a true champion of Parkinson’s. I am very familiar with vitamin B1 (thiamine), HDTT, and have read much of the dialog about it for years. I have done the taper up with B1 three times, starting at 100 mg/day, move to 200 mg/day, and after getting to 500 mg/day, simply to say the tremor in my arm went wild. Stopped for a few weeks, repeated the taper up, and the same thing happened again (and again). And I made sure to get B1 in the HCl form. So I have settled on 100 mg of B1 in the morning and 100 mg of B1 in the evening. And it helps me to take magnesium threonate twice/day alongside the B1. It always seemed to me that there is some variability in response to HDTT, which has always confused me. It did not work for me, but I am happy to know it works for many others with Parkinson’s. Good luck to your sister with HDTT. Best wishes, Frank
LikeLike
hey there – interesting read and blog overall. I saw the note regarding interaction of PEA with carnitine/ALA.
What study was that based on ? I tried to find something on the topic and actually found some studies that positively described the cominbation of either PEA with caranitine or ALA.
LikeLiked by 1 person
Let me look into the PEA/carnitine/ALA interaction. We have been out of town for a family wedding, heading home today.
LikeLike