“In all human affairs there are efforts, and there are results, and the strength of the effort is the measure of the result.” James Allen
“Storms make trees take deeper roots.” Dolly Parton
Introduction: In the presence of Parkinson’s, each person encounters a different invader that can progress very slowly or evolves quickly. Symptoms expressed are typically from the motor side of the disorder; however, the problematic non-motor disturbances can contribute to substantial morbidity. Parkinson’s can occur in younger adults, but more typically, it appears in older adults.
Nevertheless, people (person)-with-Parkinson’s (PwP) are united by the frequent occurrence of the disorder under all circumstances. We are further unified by Parkinson’s and its effect on our lives, regardless of its penetrance, severity, symptoms expressed visibly, and speed of progression. This post summarizes six pillars of Parkinson’s; another way to describe the blog post is to give six ways to take control of your Parkinson’s.
*Six Ways to Better Manage Your Parkinson’s: Before diving into ways to live with Parkinson’s, one assumption I made was that you have a functional working relationship with a Movement Disorder Specialist, Neurologist, or knowledgeable primary care physician. Having an informed conversation with your healthcare provider, the kind of therapy (and why) prescribed, and details about Parkinson’s are very relevant and vital. Thus, a functional healthcare provider represents a critical pillar on its own.
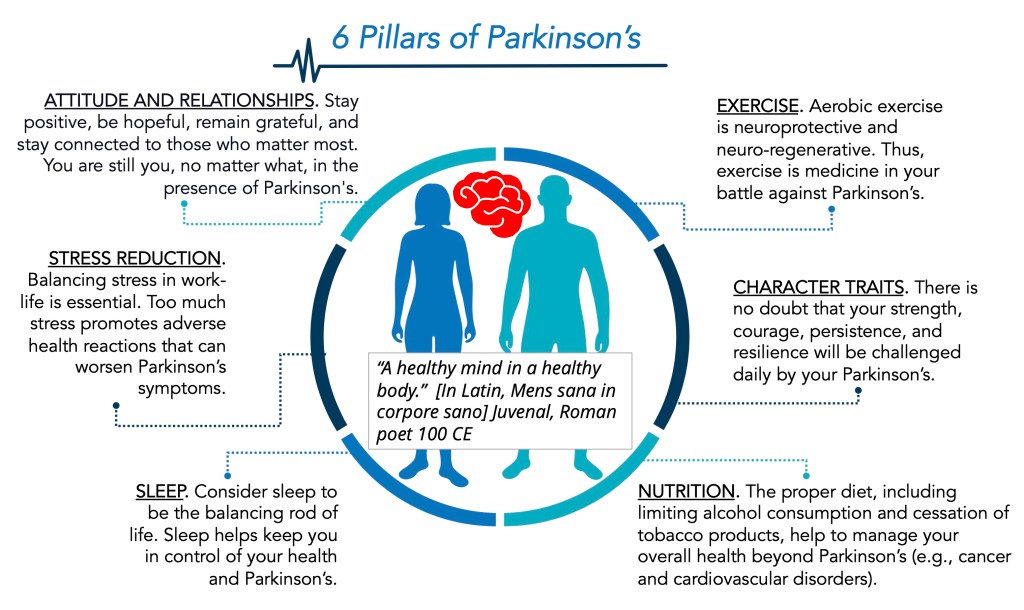
In developing the six pillars of Parkinson’s, I began by thinking about what was important thematically in this blog. It came down to six themes/ideas (given alphabetically): adapting, attitude, character traits, decisions, education, and managing life with Parkinson’s. Therefore, from my own perspective, I am pleased to present six ways to take control of your Parkinson’s. Below the schematic drawing is a more detailed description of the pillars of Parkinson’s, namely: Exercise, Character Traits, Nutrition, Sleep, Stress Reduction, and Attitude and Relationships. At the end of the blog post are the relevant blog posts regarding each of the six pillars, publications, and additional helpful links.
“Whatever is in me is stronger than what is out there to defeat me.” Caroline Myss
EXERCISE. Aerobic exercise is neuroprotective and neuro-regenerative. Thus, exercise is medicine in your battle against Parkinson’s.
Exercise is Medicine for Parkinson’s– And in every conceivable manner, it should be part of your treatment plan for Parkinson’s. For several years, animal models of Parkinson’s, when tested by exercise, have shown dramatic reversal of symptoms. In the past several years, similar results have been shown in small clinical trials.
Defining Exercise– Exercise is a physical activity that requires effort and is usually carried out to sustain or improve health and fitness. Low-intensity exercise increases your heart rate to 40-50% of your maximum heart rate (MHR), such as walking the pet dog or up several flights of steps instead of taking the elevator. Moderate-intensity exercise increases your heart rate to 50-70% MHR. High-intensity exercise increases your heart rate to 70-80% MHR. For Parkinson’s, ideally, moderate-intensity exercise for 20-30 min, 3 days per week, would be considered ideal for a PwP.
I use the acronym “FAR” to describe the type(s) of exercise one could consider for better managing Parkinson’s. FAR = Flexibility, Aerobic, Resistance:
Flexibility (and stretching) to reduce rigidity and postural instability.
Aerobic activity adds to the potential benefit of neuroprotection.
Resistance exercises help build strength and add support.
There is evidence that PwP who exercised for 2.5 hrs/week showed a smaller decline in mobility and quality-of-life over a 2 yr period.
Go FAR in your exercise program to challenge your Parkinson’s.
Neuroprotection and Neuroplasticity– Scientifically, there are two issues regarding exercise and Parkinson’s: exercise’s role in neuroprotection and exercise’s role in neuroplasticity. Several studies have shown that sustained moderate exercise can likely reduce neuroinflammation, which would be a neuroprotective effect. The main benefit of exercise for PwP is improving the quality of life and, likely, reducing neuroinflammation. Neuroplasticity is the ability of brain cells to change and form new connections, and exercise has promoted neuroplastic changes in animal models and, very recently, some evidence in human studies. Finding the most helpful biological markers to indicate neuroplastic differences remain a challenge. However, the evidence points to moderate exercise being neuroprotective and sustained exercise may promote neuroplastic changes. It is all good news. Exercise is medicine for Parkinson’s.
We now know that exercise and physical activity improve the aging processes in older adults. The Active People, Healthy Nation™ recommendation includes 150-300 minutes/week of moderate-intensity exercise or 75-150 minutes/week of high-intensity aerobic activity. Persistent moderate-intensity exercise by PwP is a sound strategy to maintain the quality of life and likely reduce neuroinflammation. Using more demanding moderate- to high-intensity exercise programs (examples include PWR!Moves, Rock Steady Boxing, Dance for PD, stationary bike, and power-walking with walking poles), with sustained use, could eventually promote neuroplasticity in PwP.
“Never say never, because limits, like fears, are often just an illusion.” Michael Jordan
CHARACTER TRAITS. There is no doubt that your strength, courage, persistence, and resilience will be challenged daily by your Parkinson’s.
The Challenge of Parkinson’s– Your life with Parkinson’s comes with challenges and obstacles. They may slowly arise, although they may eventually perturb your quality of life, possibly your livelihood (job and/or career-wise), and interfere with your daily life. Add sadly, until there is a cure, these changes are inevitable. As described earlier, each PwP has its own unique disorder, so one could not predict what these life-altering changes may be. But the battle from within against Parkinson’s is life-long, and it will never take a break or vacation. But some character traits can be effectively used against this internal scourge.
Persistence, Courage, Resilience, and Strength- I once said about persistence, “Our most difficult life challenges could create the most significant time of our lives. As President Coolidge remarked, ‘Nothing in the world can take the place of persistence; this tells me we must always keep going in dealing with our disorder. Doubtless, this is a challenging situation having Parkinson’s, but being persistent is not giving up without trying. Staying persistent creates new options and requires courage in one’s convictions.”
Likewise, I also said about courage, “Living with Parkinson’s takes courage because your enemy is within you, and you always feel its presence. Thus, your hourly-daily-effort to live-fully is a measure of your courage.”
Furthermore, I remarked that “resilience and Parkinson’s go hand-in-hand. Parkinson’s is an accumulating curse that grows slowly and is trying to dominate you. But your willpower, determination, and resilience prevent Parkinson’s from taking over completely. So stay the course, and follow your path. You will find strength in your capacity to resist and ultimately react to the challenge of Parkinson’s. Likewise, resilience will allow you to recover from the negativity of Parkinson’s.“
Part of a mantra went as follows, “Strength is found in each of us. For those of us with Parkinson’s, we use our personal character strengths to bolster our hope, courage, mindfulness/contentment/gratitude, determination, and will to survive.“
Here are Some Other ways to Deal with Parkinson’s– Sometimes, Parkinson’s has been uninvited to the party when Susan needs to have a conversation. Separate yourself for a few moments from Parkinson’s, partition it away, lock your disorder in an imaginary closet, and see if that works.
I remember being in line at Whole Foods grocery one evening, closer to the off-period than on-time, and my tremor started acting up. I tried to calm my mind with a quick mindfulness moment and relaxation while standing in line. It worked. I got through the checkout, got home, and took my drugs on schedule.
I learned a trick from a therapist whose mother has an essential tremor. She said to push hard in several directions for a few seconds on the affected limb while resisting strongly with that limb, towards and away from the body with your other hand and arm. Press hard. And for me, many times, it calms the tremor down on my arm.
“Don’t let one cloud obliterate the whole sky.” Anais Nin
NUTRITION. The proper diet, including limiting alcohol consumption and cessation of tobacco products, help to manage your overall health beyond Parkinson’s (e.g., cancer and cardiovascular disorders).
Historical Perspective of Nutrition– I begin this section with historical quotes (food, diet, and nourishment are highlighted here for effect).
Hippocrates said, “If we could give every individual the right amount of nourishment and exercise, not too little and not too much, we would have found the safest way to health.”
Hippocrates also said, “Our food should be our medicine and our medicine should be our food.”
Dr. William Harvey “Only by understanding the wisdom of natural foods and their effects on the body, shall we attain mastery of disease and pain, which shall enable us to relieve the burden of mankind.”
Dr. William Oslersaid, “Patients should have rest, food, fresh air, and exercise – the quadrangle of health.”
An ancient Ayurvedic Proverb, “When diet is wrong medicine is of no use. When diet is correct medicine is of no need.’’
Lucretius (99 B.C.-55 BC) said, ‘What is food to one man may be fierce poison to others.’’
Is there a special diet for Parkinson’s– It depends. From what I read, there is no ‘special diet’ for Parkinson’s, but there are some suggestions. However, many suggestions are available to help you live better with Parkinson’s through a nutrition plan. If the quotes above tell you anything, a proper diet will improve your health. And we have known about it for centuries. I would certainly agree with the suggestion to follow the Mediterranean Diet because it seems an ideal diet that many healthcare people and nutrition experts endorse.
In searching for the ‘ideal’ diet for Parkinson’s, one can find many suggestions on what you should eat, what you might occasionally eat, and what you should not eat. But I believe this list to be worthwhile, and one could consider living a cleaner and leaner diet.
•Follow the Mediterranean diet and use some simple food rules.
•Foods to eat frequently include (listed alphabetically) fruits, nuts, olive oil, plant-based foods, vegetables, and whole grains.
•Foods that can occasionally be present in your diet include (listed alphabetically) chicken/turkey, dairy products, eggs, and seafood.
•Foods that should only eat on special occasions include cakes/candy/cookies/pies and red meat.
•Foods to avoid are processed foods, food rich in saturated fats, sugary-rich foods, and wasted calorie drinks like orange juice.
•Since constipation is frequent in Parkinson’s, eating foods high in fiber makes sense.
•Reduce intake of sweets/desserts but eat a lot of fruits, vegetables, and grains.
Alcohol and Tobacco Products– Most of us, as we age, are susceptible to other diseases like cancer and cardiovascular disorders. I am not here to tell you about the evils of alcohol and smoking products. I am suggesting that for your health, drink only moderately and give up (if possible) smoking. We are all trying to live the best life possible in the presence of Parkinson’s, and prudence and moderation are the rules here. The Mediterranean diet is heart-healthy, and what’s good for your heart is good for your brain. Luckily, my parents cured me of smoking, so I thank them for not giving me that vice. If you smoke, try to quit. Your body and your brain will be thankful.
Diet, Alcohol, and Smoking– As always, talk this over with your family and Neurologist. We live all over the world, with different cultures, environments, and traditions; however, we share the same disorder. If your diet is working, good for you. These are guidelines about your nutritional needs, not rules to follow. The comments on alcohol and tobacco use are there for you to consider because other deadly disorders potentially percolate below the surface. Remember the advice of Zero Dean, “Healthy habits harbor happiness.”
“Strength and growth come only through continuous effort and struggle.” Napoleon Hill
SLEEP. Consider sleep to be the balancing rod of life. Sleep helps keep you in control of your health and Parkinson’s.
Sleep is a critical element of everyone’s health. Unfortunately, sleep disturbances and daytime sleepiness are common in Parkinson’s. The quality and amount of sleep can alter your well-being, and daytime fatigue can be detrimental to your vehicle safety. Notably, many PwP will have sleep problems but not report it to their healthcare provider. Thus, it is essential to understand each individual’s PwP and sleep problems because some help, understanding, and treatment are available.
Why We Need Sleep- We are not like Mr. Spock from Star Trek, the TV show of the 1960s, who required essentially no sleep. By contrast, the average human spends about a third of their life sleeping. This crucial downtime augments and bolsters the immune system and reinforces growth and development. I once noted, “The brain is like a sponge that fills up all day with fluid; sleep allows the brain to drain, renew, and fire up strong upon waking; sleep is an excellent thing.”
The Stages of Sleep– Your brain is not sleeping while you are asleep. It cycles between rapid-eye movement (REM) and non-rapid-eye movement (NREM). NREM sleep is further divided into three stages. Stage 1 is a transition time between wakefulness and sleep. Stage 2, you are preparing for deep sleep, and your heart rate slows, and your body temperature drops. The 3rd stage is deep sleep. Deep sleep is the stage where all of the body benefits happen, the stage of healing and regeneration. Your heart rate, breathing, and body temperature reach their lowest points at this stage. In REM sleep, this is your period of dreaming. You do not move in REM sleep. This is because your muscles are not receiving brain signals, called sleep atonia. By contrast, REM sleep behavior disorder (RBD) is a big problem in PwP. In RBD, a PwP will move and act out their dreams.
Sleep Debt– Likely before Parkinson’s, you slept and needed a set number of hours each night, and usually, you achieved it. However, our society today is active, and possibly, you were somewhat sleep-deprived at times from your lifestyle. PwP, for many reasons, do not sleep as much as before Parkinson’s, and they get sleep debt. You must repay this debt. Sleep debt contributes to daytime sleepiness, impaired reaction time (think of driving your car under these conditions), and impaired cognition and judgment (think of work situations in this setting). However, it is more critical for the PwP to get a good night’s sleep rather than stressing about the total number of hours slept.
Parkinson’s and Therapy Negatively Contribute to Sleep Problems– Parkinson’s related motor symptoms can alter sleep patterns like tremor motion and difficulty turning over in bed. In addition, a PwP may have impaired voluntary movement (akinesia), abnormal muscle tone that results in muscular spasms and abnormal posture (dystonia), and painful cramps. All of the above would alter your sleep pattern. Furthermore, therapy-related disruption of sleep from legitimate Parkinson’s drugs can occur. For example, there are many known side effects of the ‘gold-standard’ treatment of levodopa/carbidopa, including difficulty falling asleep or staying asleep.
Your Neurologist Needs to Understand Your Sleeping Pattern– Several general patterns can affect PwP regarding sleep dysfunction: Insomnia, Sleep Apnea, Restless Leg Syndrome, and REM Sleep Behavior Disorder. Each aspect can have treatment strategies once your healthcare provider has heard from you. Diagnosis of one or more of these problems can result in an action plan, therapy to help you sleep better, and advice on improving your sleep pattern.
“Good timber does not grow with ease; the stronger the wind, the stronger the trees” J. Willard Marriott
STRESS REDUCTION. Balancing stress in work-life is essential. Too much stress promotes adverse health reactions that can worsen Parkinson’s symptoms.
Stress is a Function of Our Life. We somehow manage life and seem to exist just fine under stress. Not really. I remember thinking I could handle a lot of stress from work; it was just part of my work world. In hindsight, it would have been far healthier to say I can not handle much stress and strive to continue to live that way.
Consequences of Stress– Chronic stress is harmful to anyone but can significantly damage those with Parkinson’s. Chronic stress can accelerate the symptoms of Parkinson’s. One could devise strategies to better deal with stress as it happens, including mindfulness meditation. From my perspective, attempting to identify the cause of stress in your life is step one. The next step is how possibly to reduce the stress. Third, finding the correct method or technique allows one to (attempt to) manage stress effectively. Finally, knowing how harmful chronic stress is in Parkinson’s, we must develop the skill to identify, manage, and hopefully eliminate repetitive stress cycles in our life.
It is difficult to suggest changing jobs to reduce stress if you have Parkinson’s. However, it is even harder to say one should retire to eliminate work-related stress for someone with Parkinson’s. Careers can span decades, and changing jobs is sometimes neither feasible nor possible. And not everyone has the luxury that I was presented with at the University to follow a 3-year phased retirement plan. Nevertheless, it prepared me somewhat for what retirement would bring. It immediately eliminated a fair amount of stress because I went from being a full-time employee to a 1/2 time professor.
Managing Stress, Life, and Parkinson’s– Living with chronic stress is detrimental to us all, but piled on top of Parkinson’s creates a hostile scenario that favors Parkinson’s. Try to find ways to reduce chronic stress because it will make a difference in your life with Parkinson’s. It really will.
“Success is achieved by developing our strengths, not by eliminating our weaknesses.” Marilyn vos Savant
ATTITUDE AND RELATIONSHIPS. Stay positive, be hopeful, remain grateful, and stay connected to those who matter most. You are still you, no matter what, in the presence of Parkinson’s.
There are many types of attitudes, some favorable and some unfavorable. Living with a progressive and chronic neurodegenerative disorder like Parkinson’s is challenging. But occasionally, so is life. My approach to Parkinson’s is that it is an enemy within that is relentless in pursuit of my brain and body. Therefore, I will do whatever I can to slow its invasion in me. However, I am steadfast in being positive, believing in hope, and remaining grateful. My glass must remain half-full in this pursuit of this menace named Parkinson’s.
About Managing Life– I once said, “You will have good and bad days, happy and sad moments, and feel healthy and sick sometimes, whether or not you have Parkinson’s. It is your decision how best to manage your Parkinson’s. However, staying focused, positive, hopeful, and informed/educated with a dose of persistence offers a path to take charge. You cannot give back your Parkinson’s; there is no two-way street. So accept it, and live with it because you still matter to the world around you.“
On Staying Positive in the Face of Parkinson’s- I said, “We balance our personal rheostat between life and career, family and friends, and service and other activities. Living positively will undoubtedly augment your meaningful life.”
Trying to Stay Hopeful Amid Parkinson’s– Hope is essential. As H.G. Wells wrote, “I hope, or I could not live.” In trying to remain optimistic and full of hope, I wrote, “Hope is a keyword in your life with Parkinson’s. A heart that feels hope keeps the body strong. A person that stays hopeful sustains their life for better-healthier moments.”
Remaining Grateful all the While With Parkinson’s– No, I am not thankful for having Parkinson’s, although it has given me a new outlook on life and a new path to follow. However, I am very grateful to many people who have enriched my life. And I am thankful for many other things I could have never imagined. Regarding gratitude, I said, “Live your life with a foundation of gratitude underneath you; it reinforces all that is good with your life today.”
Relationships Matter- Behind you is a support team, likely/hopefully, composed of the people you care about most. We accumulate friends over our lifetime, but we likely only have a few that remain essential to us. We may also have a partner/spouse necessary to our life. Cherish this person. From here, you may also have children and grandchildren. Only you can know the wealth they are to your life. Friends and colleagues may also be part of your collective family. Good for you.
Share your caring and gratitude with all of these people. We are programmed to be in relationships, and the functionality of these links will bolster your response to Parkinson’s. I see relationships as akin to a firewall providing added padding for the battle with this disorder. In thinking about the value of friendships, I said, “The bottom line is that friends are there for you when needed, and real friends will repeatedly respond when asked or challenged for assistance, advice, or a supportive smile or hug.”
Keep Living– Trying to live with Parkinson’s entirely is your goal, right? If it is working for you, good, keep going. I said about living with Parkinson’s, “We follow a path that favors happiness in the background of certain/uncertain Parkinson’s progression. We stay positive, we remain determined, and always with perseverance, we stand firm. Finally, combined with hope, we continue, we live, we continue to live, and we continue to live well and strong in the presence of Parkinson’s.”
Stay You– A constant theme in this blog, from the first post in 2015, is that no matter what happens with your Parkinson’s, you are still you. The motor and non-motor symptoms can alter us, but they cannot undo us. So stay the course, keep trying, and do not give up. Stay you.
“You have to remember that the hard days are what make you stronger. The bad days make you realize what a good day is. If you never had any bad days, you would never have that sense of accomplishment!” Aly Raisman
*Medical Disclaimer: As with anything you read here, please consult your Neurologist before changing anything related to the abovementioned points. While they all appear safe and doable, that does not mean it is suitable for your Parkinson’s.
Representative Blog Posts and References:
Exercise–
Exercise and Neuroprotection in Human Parkinson’s: The Long and Winding Road
Persistent Exercise and Physical Therapy Improve Motor and Non-Motor Symptoms of Parkinson’s
Reflection on Friday- Exercise is Medicine
Playing Golf in the Presence of Parkinson’s and Some Motivational Quotes for Exercise
Go FAR and Be ADEPT With Exercises For Parkinson’s
2019 Parkinson’s Awareness Month- 12 Rules of Life With Exercise
2019 Parkinson’s Awareness Month (Part 2)- Exercise
Parkinson’s Awareness Month: The Science Behind How Exercise Slows Disease Progression
9 Things to Know About Exercise-induced Neuroplasticity in Human Parkinson’s
Meditation, Yoga, and Exercise in Parkinson’s
Hall, M.-F.E., and F.C. Church. Integrative Medicine and Health Therapy for Parkinson Disease. Topics in Geriatric Rehabilitation 36.3 (2020): 176-186. https://bit.ly/3kIDY2K
Hall,M.-F.E., and F.C. Church. Exercise for Older Adults Improves the Quality of Life in Parkinson’s Disease and Potentially Enhances the Immune Response to COVID-19. Brain Sciences 10.9 (2020): 612. https://www.mdpi.com/2076-3425/10/9/612
Bliss, R.R. and F.C. Church. Golf as a Physical Activity to Potentially Reduce the Risk of Falls in Older Adults with Parkinson’s Disease. Sports (2021): 9, 72. https://doi.org/10.3390/sports9060072
Character Traits-
11 Tips And Character Traits For Living Better With Parkinson’s
Personal Strengths of Character
Living Well With Parkinson’s
Parkinson’s Life Strengths
Living and Working with “HOPE” in the Presence of Parkinson’s
6 Personal Strengths for Living Decisively with Parkinson’s
Word for Wednesday: Courage
Hope, Courage, Persistence, Positivity, Mindfulness, And The Journey
Word for Wednesday: Persistence
64 Quotes on Persistence to Help Your Journey With Parkinson’s Disease
Persistence and Parkinson’s
Word for Wednesday: Resilience
10 Things For A Better Life With Parkinson’s
Nutrition–
Diet & Nutrition (click here)
Diet and Nutrition (click here)
Jackson, Aeja, Christopher B. Forsyth, Maliha Shaikh, Robin M. Voigt, Phillip A. Engen, Vivian Ramirez, and Ali Keshavarzian. “Diet in Parkinson’s disease: critical role for the microbiome.” Frontiers in neurology 10 (2019): 1245.
Ma, Chaoran, Yesong Liu, Samantha Neumann, and Xiang Gao. “Nicotine from cigarette smoking and diet and Parkinson disease: a review.” Translational neurodegeneration 6, no. 1 (2017): 1-7.
Gątarek, Paulina, and Joanna Kałużna-Czaplińska. “Nutritional aspects in Parkinson’s disease.” Critical Reviews in Food Science and Nutrition 62, no. 23 (2022): 6467-6484.
Sleep–
Sleep Disturbances in Parkinson’s and the Eagles Best Song Lyrics
Part 3: Journey to Parkinson’s and Polysomnography (Sleep Study)
Stefani, Ambra, and Birgit Högl. “Sleep in Parkinson’s disease.” Neuropsychopharmacology 45, no. 1 (2020): 121-128.
Körner, Yvonne, Charlotte Meindorfner, Jens Carsten Möller, Karin Stiasny‐Kolster, Doris Haja, Werner Cassel, Wolfgang Hermann Oertel, and Hans‐Peter Krüger. “Predictors of sudden onset of sleep in Parkinson’s disease.” Movement Disorders: Official Journal of the Movement Disorder Society 19, no. 11 (2004): 1298-1305.
Zahed, Hengameh, Jose Rafael Pantoja Zuzuarregui, Ro’ee Gilron, Timothy Denison, Philip A. Starr, and Simon Little. “The neurophysiology of sleep in Parkinson’s disease.” Movement Disorders 36, no. 7 (2021): 1526-1542.
Stress Reduction-
Living Better with Parkinson’s
Wellness Checklist for Life in the Presence of Parkinson’s
Journey with Parkinson’s: Managing Daily Life
Tuijt, Remco, Aylin Tan, Megan Armstrong, Jennifer Pigott, Joy Read, Nathan Davies, Kate Walters, and Anette Schrag. “Self-management components as experienced by people with Parkinson’s disease and their carers: a systematic review and synthesis of the qualitative literature.” Parkinson’s Disease 2020 (2020).
Committee, G.P.s.D.S.S. Factors impacting on quality of life in Parkinson’s disease: results from an international survey. Movement Disorders 2002, 17, 60-67.
Kuhlman, G.D.; Flanigan, J.L.; Sperling, S.A.; Barrett, M.J. Predictors of health-related quality of life in Parkinson’s disease. Parkinsonism & Related Disorders 2019, 65, 86-90, doi:https://doi.org/10.1016/j.parkreldis.2019.05.009.
Tuijt, R.; Tan, A.; Armstrong, M.; Pigott, J.; Read, J.; Davies, N.; Walters, K.; Schrag, A. Self-Management Components as Experienced by People with Parkinson’s Disease and Their Carers: A Systematic Review and Synthesis of the Qualitative Literature. Parkinson’s Disease 2020, 2020, 8857385, doi:10.1155/2020/8857385.
Attitude and Relationships-
The Positive Impact of Friends: Journey with Parkinson’s
Staying Positive With Parkinson’s
Understanding The Positive Health Benefits of Gratitude
Positively Parkinson’s
World Parkinson’s Day 2022: Hope Has Not Been Canceled
Words with Hope
Thought for Thursday: Live With Hope
Staying Hopeful With Parkinson’s
Hope- 2019 Parkinson’s Awareness Month
Hope in the Presence of Parkinson’s
Hope, Courage, Persistence, Positivity, Mindfulness, And The Journey
Hope Resides Within the Adversity of Parkinson’s
The Attitude of Gratitude in the Presence of Parkinson’s
Thought for Thursday: With A Little Help From My Friends
Word for Wednesday: Gratitude
Parkinson’s: Reflective Gratitude of Life
Brief Report: Contentment, Gratitude, and Mindfulness in the Presence of Parkinson’s
Understanding The Positive Health Benefits of Gratitude
Cover Photo Image by Joshua Choate from Pixabay



One Reply to “”